LC-MS Method for Studying the Pharmacokinetics and Bioequivalence of Clonidine Hydrochloride in Healthy Male Volunteers
-
 Danafar, Hossein
Department of Medicinal Chemistry, Faculty of Pharmacy, Zanjan University of Medical Sciences, Zanjan, Iran, Tel: +98 241 4273638, E-mail: danafar@zums.ac.ir
Danafar, Hossein
Department of Medicinal Chemistry, Faculty of Pharmacy, Zanjan University of Medical Sciences, Zanjan, Iran, Tel: +98 241 4273638, E-mail: danafar@zums.ac.ir
-
Zanjan Pharmaceutical Nanotechnology Research Center, Zanjan University of Medical Sciences, Zanjan, Iran
-
Department of Medicinal Chemistry, Faculty of Pharmacy, Zanjan University of Medical Sciences, Zanjan, Iran
-
Hamidi, Mehrdad
-
Zanjan Pharmaceutical Nanotechnology Research Center, Zanjan University of Medical Sciences, Zanjan, Iran
-
Department of Pharmaceutics, Faculty of Pharmacy, Zanjan University of Medical Sciences, Zanjan, Iran
Abstract: Background: A simple and sensitive high performance liquid chromatography-electrospray ionization mass spectrometry method has been evaluated for the assignment of clonidine hydrochloride in human plasma.
Methods: The mobile phase composed of acetonitrile-water 60:40 (v/v) and 0.2% formic acid 20 µl of sample was chromatographically analyzed using a repacked ZORBAX-XDB-ODS C18 column (2.1 mmx30 mm, 3.5 μ). Detection of analytes was achieved by tandem mass spectrometry with Electrospray Ionization (ESI) interface in positive ion mode operated under the multiple-reaction monitoring mode (m/z 230.0 →213). Sample pretreatment consisted of a one-step Protein Precipitation (PPT) with methanol and perchloric acid (HClO4) of 0.10 ml plasma.
Results: Standard curve was linear (r=0.998) over the concentration range of 0.01-10.0 ng/ml and showed suitable accuracy and precision. The Limit of Quantification (LOQ) was 0.01 ng/ml. The mean (SD) Cmax, Tmax, AUC0–t and AUC0–∞ values after administration of the test and reference formulations, respectively, were in this manner: 6.16 (0.32) versus 6.21 (0.07) ng/ml, 30.12 (0.86) versus 30.13 (0.73) hr, 290.37 (1.13) versus 293.39 (1.22) ng/ml/hr, and 350.17 (1.98) versus 352.96 (1.67) ng/ml/hr. The mean (SD) t1/2 was 120.12 (1.90) hr for the test formulation and 120.96 (1.54) hr for the reference formulation. No statistical differences were showed for Cmax and the area under the plasma concentration-time curve for test and reference tablets.
Conclusion: The method is rapid, simple, very steady and precise for the separation, assignment, pharmacokinetic and bioavailability evaluation of clonidine in healthy Iranian adult male volunteers.
Introduction :
Clonidine, an imidazoline derivative, is a centrally acting hypotensive agent but its use is being explored in a number of other indications such as anesthesia and the management of opiate withdrawal (Figure 1)1. Clonidine belongs to a class of drugs called central alpha-adrenergic agonists. Clonidine has been in clinical use for over 40 years, which is used to treat hypertensive disorders, hyperactivity disorder, anxiety disorders, migraine, menopausal flushing and certain pain conditions 1. It has been proven by clinical studies that fluctuation of clonidine plasma concentration is responsible for its side effects. Then, a sensitive and reliable analytical method is needed to be established to describe the pharmacokinetic properties of clonidine in clinical trials thoroughly 2,3. Several bio analytical methods are reported to determine the presence of clonidine in different biological matrices like plasma 4,5, serum 6,7,11-13, urine 6, and cerebrospinal fluids 2. Sensitive and selective methods are based on LC–MS/MS 3-5,7,8,13, HPLC 2,9,10,12,14, GC–MS 11 and capillary isotachophoresis 6. Muller et al 15 developed LC-MS/MS method in human serum with a Lower Limit of Quantitation (LLOQ) of 0.1 ng/ml while Li et al 16 developed a 2D strong action exchange reversed-phase LC-MS/MS method in dried blood spots with an LLOQ of 0.1 ng/ml. Although these methods were sufficiently sensitive, they were not suitable for most laboratories to perform studies involving high through-put samples for therapeutic monitoring. Meanwhile, a high-throughput validated analytical method 17 for the quantitation of clonidine using LC-MS/MS has been published with a calibration range of 0.05-2.50 ng/ml using 500 μl plasma. However, this study involved a solid-phase extraction, which was costly. Most often, these methods utilize solid phase extraction for sample cleanup. Since most of these methods were developed for human samples, relatively large volumes (i.e. >0.1 ml) of plasma were needed to achieve the desired sensitivity limit. There are a limited number of methods reported for the quantitation of clonidine in preclinical samples. Measurement of clonidine in human plasma by LC/MS/MS has yielded improved sensitivity limits of 0.5 ng/ml, and a liquid-liquid extraction procedure, and 5 ng/ml, a solid-phase extraction procedure. Therefore, it is valuable to describe the pharmacokinetic properties of clonidine to support in vivo pharmacokinetic study of clonidine. Our previous work was determination of presence of drug by LC-MS and HPLC methods in human plasma 18-21. In the present study, a simple, selective and high-throughput method was described using high performance liquid chromatography coupled with electrospray ionization single quadruple mass spectrometry for the estimation of clonidine in human plasma for therapeutic drug monitoring and pharmacokinetic studies.
Materials and Methods :
Materials: Clonidine hydrochloride extended release test tablets (Batch no. 88001, Tolyd Daroo), clonidine hydrochloride reference tablets (Batch no. 819609, (Boehringer Ingelheim) amended by EC (European Community) and clonidine hydrochloride reference standard (99.9% purity) were supplied and identified by Boehringer Ingelheim pharm. Acetonitrile was HPLC grade and was purchased from Merck (Merck Company, Germany). Other chemicals and solvents were of analytical or chemical lab purity grades, as needed and purchased.
Instrumentation and operating conditions
Liquid chromatography: Liquid chromatography was carried out using a High Performance Liquid Chromatography (HPLC) system (Agilent Technologies, model LC-1200, Englewood, USA) equipped by an auto sampler. The analytical column used was a C18 column (Company, ZORBAX- XDB-ODS, USA) (2.1 mmx30 mm, 3.5 μ) and was operated at 250ºC. The mobile phase consisted of acetonitrile-water 60:40 (v/v) and 0.2% formic acid was set at a flow rate of 0.2 ml/min.
Mass spectrometry: Mass Spectrometric (MS) detection was performed using a triple-quadruple mass spectrometer (Agilent Technologies, model LCMS-6410, Englewood, USA) with an Electrospray Ionization (ESI) interface. The ESI source was set at positive ionization mode. The (M +H)+ m/z 230 for clonidine was selected as detecting ions (m/z 230.0 →213). The MS operating conditions were optimized as follows: Ion spray voltage was set to 4000 V, temperature of the ion transfer capillary was 250oC, Nebulizer gas (NEB) was 10 and Curtain gas (CUR) was 8. The quantification was performed via peak-area. Data acquisition and processing were accomplished using agilent LC/MS/MS solution Software for LC/MS/MS-6410 system.
Preparation of stock solutions: Stock solutions of clonidine hydrochloride were prepared in HPLC mobile phase at concentrations of 1 mg/ml and were stored at 4oC. Working solutions of clonidine were prepared daily in HPLC mobile phase by appropriate dilutions at 0.01, 0.05, 0.1, 0.5, 1, 2, 5, 7 and 10 ng/ml.
Sample preparation and extraction procedure: Sample pretreatment involved a one-step Protein Precipitation (PPT) with methanol and perchloric acid (HClO4). A 0.10 ml aliquot of the collected plasma sample from a human volunteer was pipetted into a 1 ml centrifuge tube and then 0.1 ml methanol and 0.1 ml HClO4 were added and then vortexed for 2 min. After centrifugation of the sample at 15400 rpm for 20 min, the organic layer was transferred to another 1 ml centrifuge tube and an aliquot of 20 µl was injected into the LC-MS system.
Standard curves: Proper volumes of one of the above-mentioned working solutions to produce the standard curve points were equivalent to 0.05, 0.20, 1.0, 5.0, 10.0, 20.0, 50.0 and 100.0 ng/ml of clonidine hydrochloride and each sample was processed as described. Finally, the nominal known plasma concentrations were plotted against the corresponding peak areas to construct the standard curve.
Preparation of quality control samples: Quality control samples were prepared daily by spiking different samples of 0.1 ml plasma each with proper volume of the corresponding standard solution to produce a final concentration equivalent to low level (0.01 ng/ml), middle level (1.0 ng/ml) and high level (10.0 ng/ml) of clonidine hydrochloride. The following procedures were the same as described above.
Method validation
Assay specificity: To evaluate the matrix effect on the ionization of analytes, five different concentration levels of clonidine (0.05, 0.20, 5.00, 10.00 and 100.00 ng/ml-1) were prepared in the drug-free blank plasma as five sample series using five different lots of the drug-free plasma and the samples were processed, as described and injected to LC-MS. The same concentrations were prepared in mobile phase instead of plasma and analyzed for drug concentration using the same procedure. A comparison of the matrix effects of the two variants was made as an indicator of the method specificity.
Linearity: Standard curves of ten concentrations of clonidine ranged 0.01-10.0 ng/ml were assayed. Blank plasma samples were analyzed to ensure the lack of interferences but not used to construct the calibration function. The Limit of Detection (LOD) was estimated from signal-to- noise ratio. This parameter was defined as the lowest concentration level resulting in a peak area of three times the baseline noise. The Limit of Quantification (LOQ) was defined as the lowest concentration level that provided a peak area with a signal-to- noise ratio higher than 5, with precision (%CV) within±20% and accuracy (%recovery) between 80% and 120% 22,23.
Within-run variations: In one run, three samples with concentrations of 0.01, 1, and 10 ng/ml (from high, middle, and low regions of the standard curve) were prepared in triplicate and analyzed by developed LC-Mass method. Then, the coefficient of variations (CV%) of the corresponding determined concentrations were calculated in each case.
Between-run variations: On three different runs, samples from upper, intermediate, and lower concentration regions used for construction of standard curve (the same as within-run variations test) were prepared and analyzed by LC-Mass method. Then, the corresponding CV% values were calculated.
Extraction recovery: Three samples with concentrations of 0.01, 1, and 10 ng/ml (from high, middle and low regions of the standard curve) were prepared in triplicate and analyzed by developed LC-Mass method. Then, the ratio of the recorded peak heights to the peak heights resulted from the direct injection of the aqueous solutions of clonidine with the same concentrations were determined as percentage in each case.
Repeatability test: To test the method repeatability, six independent spiked plasma samples with a drug concentration of 1 ng/ml were prepared as described. A single injection of each preparation was made to LC/MS and the %RSD between the results was determined as the repeatability of the method.
Intermediate precision: On a day different from that of repeatability study, a second analyst executed analysis of further six samples prepared as described in repeatability test procedure. The analysis was carried out using fresh reagents and a different HPLC column. The %RSD between six measurements was determined along with the %RSD between the total of 12 measurements from the repeatability and intermediate precision tests.
Reproducibility: Mean results for the same sample analysis between our laboratory and two different test facilities were obtained and the %difference between content measurements was calculated using the equation: [(highest value-lowest value)/mean value]x100.
Stability
Freeze and thaw stability: Three concentration levels of QC plasma samples were stored at the storage temperature (-20oC) for 24 hr and thawed unassisted at room temperature. When completely thawed, the samples were refrozen for 24 hr under the same conditions. The freeze-thaw cycle was repeated twice, then the samples were tested after three freeze (-20oC)-thaw (room temperature) cycles.
Short-term temperature stability: Three concentration levels of QC plasma samples were kept at room temperature for a period that exceeded the routine preparation time of samples (around 6 hr).
Long-term stability: Three concentration levels of QC plasma samples kept at low temperature (-20oC) were studied for a period of 4 weeks.
Post-preparative stability: The auto sampler stability was conducted reanalyzing extracted QC samples kept under the auto sampler conditions (4oC) for 12 hr.
Standard curve and quality control sample in each batch: A standard curve in each analytical run was used to calculate the concentration of clonidine in the unknown samples in the run. It was prepared at the same time as the unknown samples in the same batch and analyzed in the middle of the run. The QC samples in five duplicates at three concentrations (0.010, 1.0 and 10.0 ng/ml) were prepared and were analyzed with processed test samples at intervals per batch.
Clinical study design
Twelve male subjects were enrolled in a randomized, two-treatment, two-period, single-dose crossover study with a 3 week washout between the first dosing in period I and the first dosing of period II. Single dose study subjects fasted from the night before dosing until 2 hr after dosing for each session. For clonidine reference group, the 0.2 mg clonidine formulation was administered and blood samples were obtained prior to dose administration (time 0) and at 0.25, 0.5, 1.0, 1.5, 2.0, 3.0, 4.0, 6.0, 8.0, 10.0, 24.0, 48.0, 72.0, 96.0, 120.0, 144.0, 168.0 and 192 hr after the dose. For clonidine-test group, the 0.2 mg clonidine test formulation was administered and blood samples were obtained prior to dose administration (time 0) and at 0.25, 0.5, 1.0, 1.5, 2.0, 3.0, 4.0, 6.0, 8.0, 10.0, 24.0, 48.0, 72.0, 96.0, 120.0, 144.0, 168.0 and 192 hr after the dose. The blood samples were immediately centrifuged at 1600×g for 10 min. The plasma was removed and stored at -20oC until analysis was done.
Pharmacokinetic study: The pharmacokinetic parameters for clonidine were designed using standard non-compartmental methods. The peak serum concentration (Cmax) and the time to reach it (Tmax) were evaluated from visual examination of the data and used as criteria of the rate of absorption. The apparent elimination rate constant (β) was determined by linear regression of log-transformed data in the terminal phase of the serum concentration-time profile 24. The elimination half-life (t1/2) was considered by the quotient of 0.693/β. In addition, the area under plasma concentration time (AUC0-t) curve was determined by the linear trapezoidal rule from the measured serum concentrations from zero to the time of the last quantifiable concentration (Ct). The AUC0-i, the area under the serum concentration-time curve extrapolated to perpetuity, was designed according to the following equation 19: AUC0-∞=AUC0-t+Ct/Kel. The pharmacokinetic profiles of clonidine from two tablet formulations were compared and the comparative bioavailability of test/reference product was calculated using the ratio of AUC0-f (test)/AUC0-C (reference) 24.
Results :
Method development: Considering the complex biological matrix of the samples to be analyzed and the nature of the method to be used for drug assay, the method development efforts were made in two different areas of sample preparation and analyte separation which are discussed in detail in the following sections.
Sample preparation: Protein precipitation was necessary and important because this technique not only purifies but also concentrates the sample. Methanol, perchloric acid and acetonitrile were all attempted and methanol and perchloric acid were finally adopted because of their high extraction efficiency and less interference. Precipitation with and without adding 0.1 M NaOH (100 µl) were both tried, and obvious differences were not observed, so the precipitation using methanol, perchloric acid without adding 0.1 M NaOH was used at last.
Analyte separation: LC-MS/MS with positive ESI was selected to detect clonidine in human plasma. A prominent fragment with m/z 230.0 was observed in the product ion scan with positive ESI. The multiple-reaction monitoring (+) chromatograms extracted from supplemented plasma are depicted in figure 2. As shown, the retention time of clonidine was 2.4 min. The total HPLC-MS analysis time was 4 min per sample. A representative chromatogram of a plasma sample obtained at 6 hr from a subject who received a single oral dose (0.2 mg) is shown in figure 2C. No interferences of the analytic were observed. Figure 2A shows an HPLC chromatogram for a blank plasma sample indicating no endogenous peaks at the retention positions of clonidine. Figure 2D shows supplemented plasma and the concentration of clonidine is 4 ng/ml. All the ratios of the peak area resolved in blank sample compared with that resolved in mobile phase are between 85 and 15%, which means no matrix effect for clonidine in this method was observed.
Method validation
Assay specificity: As it is clearly evident from the typical chromatograms of the developed method shown in figure 2, there are no discernible interferences between the matrix factors and the analyst. This, in turn, ensures obtaining reliable results from the method for determination of biological concentrations of clonidine.
Linearity and LOQ: The method produced linear responses throughout the clonidine concentration range of 0.01-10 ng/ml, which is suitable for intended purposes. A typical linear regression equation of the method was: y=1444.3, x=16740, with x and y representing clonidine concentration (in ng/ml) and peak height (in arbitrary units), respectively, and the regression coefficient (r) of 0.998. The LLOQ and LOD for clonidine hydrochloride was proved to be 0.010 and 0.005 ng/ml, respectively. Figure 2B shows the chromatogram of an extracted sample that contained 0.01 ng/ml (LOQ) of clonidine hydrochloride.
Within-run variations and accuracy: The within-run variations of the developed LC-Mass method as well as the corresponding absolute recoveries are shown in table 1. These data clearly show that the developed method has an acceptable degree of repeatability and accuracy within an analytical run.
Between-run variations and accuracy: The between-run variations of the developed LC-Mass method as well as the corresponding absolute recoveries are shown in table 2. As stated for the previous test, these data clearly show that the developed method has an acceptable degree of reproducibility and accuracy between different analytical runs.
Relative recovery (Matrix effect): The extraction recovery determined for clonidine hydrochloride was shown to be consistent, precise and reproducible. Data is shown below in table 3. These data indicate that there is no significant matrix effect on the outputs of the assay method.
Repeatability test: The repeatability of the method is shown in table 4. As shown, the method has a remarkable repeatability for the drug assay in plasma.
Intermediate precision: The results of the intermediate precision test are shown in table 5. As indicated, the developed method shows an acceptable intermediate precision for clonidine hydrochloride assay.
Reproducibility: The highest test result of the spiked plasma with 1 ng/ml-1 clonidine was137854 and the lowest value was 137235 with the mean value of 137546. Therefore, the %difference was 0.45% which means a high reproducibility for the method.
Stability: Table 6 summarizes the freeze and thaw stability, short term stability, long-term stability and post-preparative stability data of clonidine hydrochloride. All the results showed the stability behavior during these tests and there were no stability related problems during the samples routine analysis for the pharmacokinetic, bioavailability or bioequivalence studies. The stability of working solutions was tested at room temperature for 6 hr based on the results obtained; these working solutions were stable within 6 hr.
Bioequivalence study: The mean serum concentration-time profiles after single oral dose administration of reference and test formulations are shown in figure 3. As it is shown, the mean serum concentration-time curves from the test and reference products are about superimposable. Furthermore, there was no important distinction between clonidine serum concentrations at each time point subsequent to oral administration of the two formulations. At the first case time (0.5 hr), the drug was computable in all subjects following the administration of both arrangements. The resulting pharmacokinetic parameters are shown in table 7. Mean maximum serum concentrations of 6.16±0.32 and 6.21±0.07 ng/ml were obtained for the test and reference formulations, respectively. Tmax, the time required to reach the maximum serum concentration, was 3.12±0.86 and 30.13±0.73 hr, respectively. Beside Cmax and Tmax, the ratio of Cmax/AUC0-∞also can be used as a parameter for determining the absorption rates in bioequivalence studies 25,26. These calculated ratios were 2.12 and 2.11% for the test and reference formulations.
The parameters used as procedures of the amount of absorption are AUC0-t and AUC0-∞. The AUC0-t and AUC0-∞ for the test formulation were 290.37±1.13 and 350.17±1.98 ngh/ml, respectively. The considered values for the reference formulation were 293.39±1.22 and 352.96±1.67 ngh/ml in the order mentioned. Both formulations were well tolerated by all the volunteers in both phases of study. No clinical adverse events occurred during the study. All calculated pharmacokinetic parameter values were in good agreement with the previously reported values. For bioequivalence evaluation, Cmax, AUC0-t and AUC0-∞ were considered as primary parameters. The mean and standard deviation of these parameters of the two formulations were found to be very close, indicating that the plasma profiles generated by test formulation are comparable to those produced by reference formulation.
This study examined the PK properties, bioavailability, and bioequivalence of test and reference products of clonidine, a newly developed dispersible tablet and an established branded tablet in healthy Iranian volunteers. These results indicated that the analytical method was linear, precise and accurate. Test and reference formulation were found to be bioequivalent. Hence, it was concluded that formulation test is bioequivalent with formulation reference.
Discussion :
An open-labeled, single-dose with food, two-treatment, two-period, two-sequence randomized two way crossover design in 12 healthy adult volunteers was considered appropriate and standard for bioequivalence evaluation of the generic and the reference products. The study simulates real life conditions including the influence of meals as well as circadian effects on the performance of the product. For a safety reason, co-administration of the drug with food can reduce nausea, a common side effect of clonidine hydrochloride. In general, the pharmacokinetic parameters for both formulations were similar to the pharmacokinetic parameters of clonidine hydrochloride in previous published data. In addition, no significant differences of the Tmax values between the two formulations were observed (p>0.05). Therefore, the two formulations of clonidine hydrochloride are considered bioequivalent in terms of the rate and extent of absorption. Moreover, both formulations were well tolerated. Hence, the test and reference formulations of clonidine hydrochloride 0.2 mg are bioequivalent.
Conclusion :
A sensitive, selective, accurate and precise HPLC method with selected ion monitoring by triple quadrupole mass spectrometer with ESI interface was developed and validated for determination of clonidine hydrochloride in human plasma. This method offers several advantages such as a rapid and simple extraction scheme and a short chromatographic run time, which make the method suitable for the analysis of large sample batches resulting from the pharmacokinetic, bioavailability or bioequivalent study of clonidine hydrochloride.
Acknowledgement :
The authors wish to thank Zahravi Pharmaceuticals (Tabriz, Iran) for kindly providing us clonidine samples. We also would like to thank Zanjan University of Medical Sciences and Iranian Blood Transfusion Organization for providing the drug-free plasma.
Figure 1. Chemical structure of clonidine.
|

Figure 2. The MRM (+) chromatograms of clonidine. A) Blank plasma, B) LOQ (concentration of clonidine=0.01 ng/ml). C) The MIM (+) chromatograms for plasma sample of a healthy volunteer; the concentration of clonidine was 1.12 ng/ml. D) Supplemented plasma (concentration of clonidine=4 ng/ml).
|
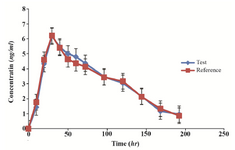
Figure 3. Comparative pharmacokinetic profile of clonidine hydrochloride following oral administration of 0.2 mg test and reference products to healthy volunteers.
|
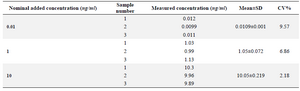
Table 1. Within–run variations and accuracy of the LC-Mass method for quantitation of clonidine hydrochloride (n=3)
|
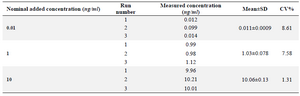
Table 2. Between–run variations and accuracy of the LC-Mass method for quantitation of clonidine hydrochloride (n=3)
|
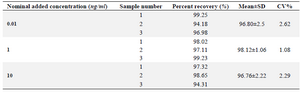
Table 3. Relative recovery of clonidine hydrochloride by the LC-Mass method (N=3)
|
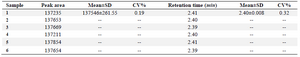
Table 4. Repeatability of the test results for spiked plasma containing 1 ng/ml-1 clonidine hydrochloride
|
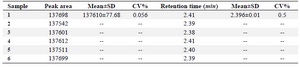
Table 5. Intermediate precision of the test results for spiked plasma containing 1 ng/ml-clonidine hydrochloride
|
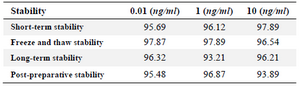
Table 6. Data showing stability of clonidine hydrochloride in human plasma at different QC levels (n=5)
Data are presented as the percentage of the remaining concentration to the initial starting concentration
|
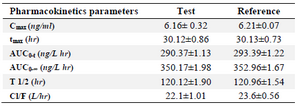
Table 7. Pharmacokinetic parameters of clonidine hydrochloride after single oral dose of the test and reference product (Mean±SD)
|
|